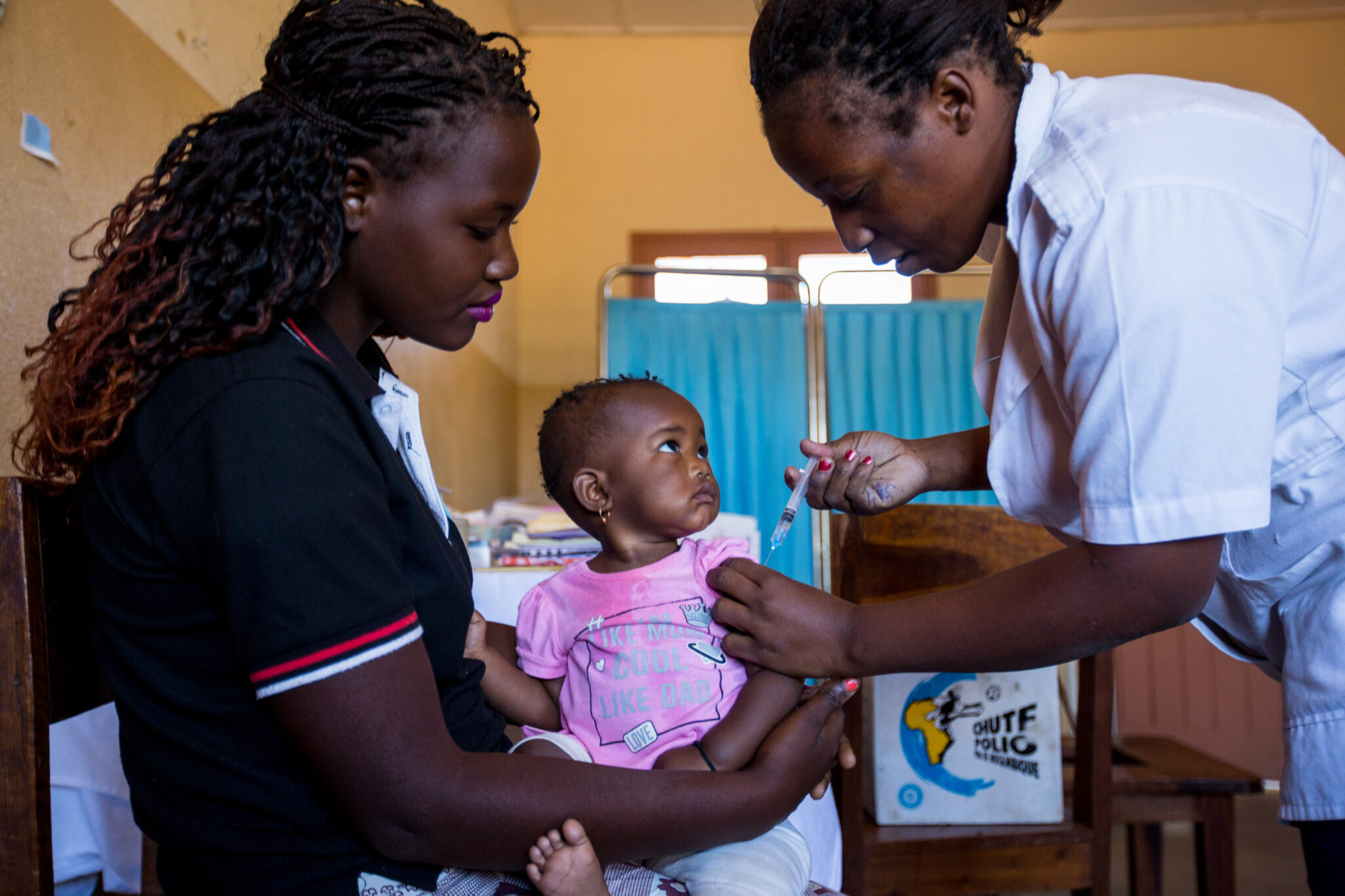
A vaccination campaign in Mozambique. (Denis Onyodi / VillageReach Photo)
While scientists have been able to manufacture and test COVID-19 vaccines in a near-unimaginable record breaking time, vaccine delivery in the US has been bumpy, slow, and unfair.
What is to blame for the chaotic rollout?
“The classic trap the US fell into … is that we didn’t put the same amount of energy into the way we wanted to deliver the vaccine that we put into the science of making the vaccine,” said Emily Bancroft, president of VillageReach, a Seattle-global health nonprofit founded in 2001 helping deliver vaccines to underserved communities.
In the eleven weeks since the first vaccines were shot into American guns, the vaccination campaign has improved significantly. Approximately 55.5 million Americans – or nearly 17% of the population – have received one or more doses of the vaccine, made by Pfizer or Moderna. Almost 9% are fully vaccinated. In Washington state, nearly 15% of the population received at least one dose, and 8.4% received two shots.
 Emily Bancroft, President of VillageReach. (VillageReach photo)
Emily Bancroft, President of VillageReach. (VillageReach photo)
But the US has gone wrong on all three key components of a successful program, Bancroft said. This includes the creation of central and local administrative plans, the preparation of a sufficient supply of medical personnel for the delivery of the recordings and the development of the data infrastructure for tracking the vaccine doses and the recipients.
Now President Biden has said the country is on track to have enough COVID vaccine “for every adult in America” by the end of May. The question is, are we ready to deliver.
Massive vaccination programs are difficult – but not impossible. In recent years, numerous African countries have launched campaigns to combat cholera, polio and measles, delivering millions of doses in a matter of days or weeks. These efforts provide lessons that Americans could learn from.
When it came to the US COVID vaccination program, “we built the car the way we drove it,” said Bancroft, “instead of stepping back a year ago and saying,“ OK, this vaccine is coming. What are the parts that will be there and how do we learn from mass vaccination campaigns in other countries? ‘“
VillageReach has a seat on technical working groups in five African countries to prepare for the introduction of COVID vaccination, which has been delayed due to the global shortage of vaccines and the fact that richer countries have picked up the starting doses. The introduction of vaccines in Mozambique begins every day. Meanwhile, two people from the nonprofit are helping the Seattle area campaign and helping out at two King County’s mass vaccination sites.
Here are some additional lessons from Bancroft on the US vaccination effort:
- In many African countries, there are community health workers who are less qualified than doctors and trained in the administration of vaccines. More recently, U.S. health organizations have trained nursing and pharmacy students and provided refresher courses to retired health care providers to increase the number of vaccines.
- In lower-income countries, healthcare systems often use simple software to manage campaigns, but even that has been lacking in the US. A VillageReach employee developed a tool to track vaccine supplies in King County based on experience in managing vaccine stocks in Africa. It predicts how many doses will be needed the next day based on previous usage to streamline operations.
- In the US, there are generally no robust community networks in Africa that can be activated to bring people to vaccination sites and share factual information about vaccines and counteract misinformation. This lack of human infrastructure has contributed to the challenge of vaccine inequalities: Racially diverse communities hardest hit by COVID also see declines in vaccination rates.
 A vaccination campaign in Mozambique. (Paul Joseph Brown / VillageReach Photo)
A vaccination campaign in Mozambique. (Paul Joseph Brown / VillageReach Photo)
The US vaccinated nearly half of the population against flu in 2019. Why was it so difficult to get COVID pictures? There are many reasons, including the need to keep the first two approved mRNA vaccines at very low temperatures, the challenge of tracking people for the two doses required, and because the vaccines are not available to everyone, but to recipients at risk Give priority.
Vaccine doses are given much faster and now the limited hurdle is the limited supply of vaccines. The U.S. Food and Drug Administration last week granted emergency approval for a third vaccine from Johnson & Johnson, which requires only one dose and should be available in the coming days.
But there is going to be another pandemic, experts warn, and long-term improvements to our health system are needed to provide a better response.
“We haven’t invested enough in our public health infrastructure in the US for a long time,” said Bancroft. “And that’s how you will see it when you try to waver about doing something as massive as this.”