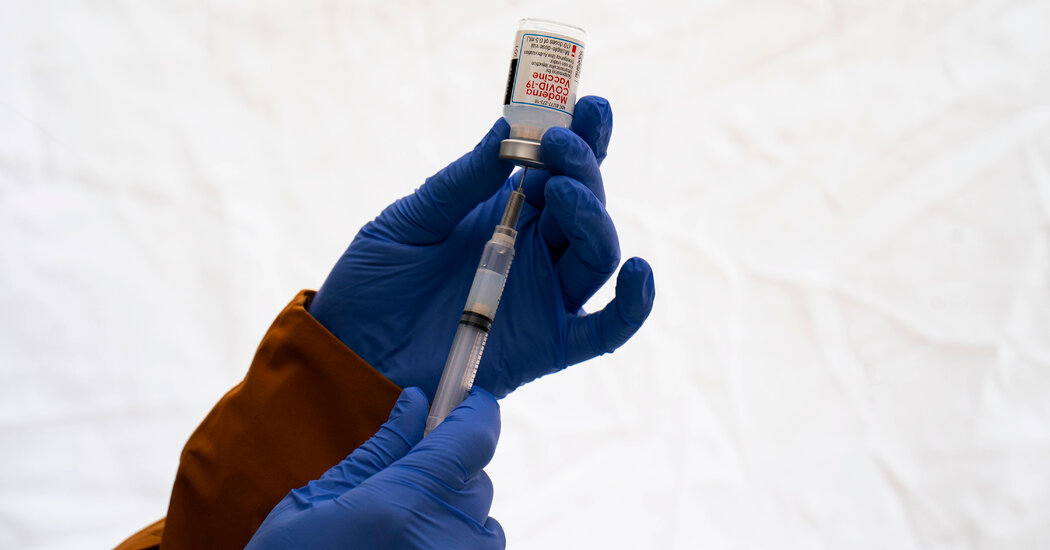
Here’s what you need to know:
Credit…Spencer Platt/Getty Images
Vaccinations in many American prisons, jails and detention centers are lagging far behind the United States as a whole, prompting public health officials to worry that these settings will remain fertile ground for frequent, fast-spreading coronavirus outbreaks for a long time to come.
Nationally, more than 60 percent of people ages 18 or older have received at least one dose of vaccine so far. But only about 40 percent of federal prison inmates, and half of those in the largest state prison systems, have done so. And in immigration detention centers, the figure is just 20 percent.
With the overall pace of vaccinations slowing in the United States — down to about 1.88 million doses a day on average, according to federal data — the Biden administration has been stepping up efforts to win over the hesitant and reach people in underserved and vulnerable communities and those facing access issues.
Over the course of the pandemic, prison inmates have been more than three times as likely as other Americans to become infected with the virus, according to a New York Times database. The virus has killed prisoners at higher rates than the general population, the data shows, and at least 2,700 have died in custody.
No racial breakdown is available for coronavirus cases in prisons, but health officials say African-Americans are likely to be overrepresented, since they account for a much larger share of inmates (33 percent) than they do of the overall population (13 percent), and the pandemic has disproportionally hit Black Americans in general.
Black and Hispanic people across the United States have received a disproportionately smaller share of vaccinations to date, according to a New York Times analysis of state-reported race and ethnicity information, though some progress has been made.
High vaccination rates in another kind of high-risk setting, nursing homes, have greatly reduced the spread of the virus there. But unlike nursing home residents, prisoners were generally not a high priority for early vaccination. By April 19, the 50 states, the District of Columbia and Puerto Rico had expanded eligibility to all adults. Still, refusal rates in prisons have been high.
Many inmates say they mistrust both the vaccine and the prison authorities who try to persuade them to get inoculated. Beyond that, some prison vaccination efforts have been hampered by mistakes.
Prison officials in some states have tried offering inmates incentives to be vaccinated, including extra food — with varying degrees of success.
Jonathan Brooks, who is incarcerated at Wake Correctional Center in North Carolina, said incentives like free phone calls and approval priority for family visits were insulting.
“That’s something that we are required to have anyway — phone calls and receiving visits from our loved ones — so to actually recommend something like that to get us to take the vaccine, I feel like that’s really a slap in the face,” he said. Mr. Brooks said he did not intend to get the vaccine.
Prison guards have also tended to be skeptical about getting vaccinated. Colorado began offering correctional officers $500 bonuses to get inoculated.
A review of seven of the largest state prison systems found a wide range in vaccination rates. Pennsylvania has gotten at least one shot into 71 percent of inmates, while neighboring New York has managed just 35 percent. In California the figure is 68 percent; in Texas, 50 percent.
Michael Carvajal, director of the federal prison system, told the Senate Judiciary Committee in April that each of the system’s 126,000 inmates would have access to the vaccine by mid-May. But as of Thursday morning, only 40 percent of inmates and 50 percent of employees had been vaccinated.
Emily Wang, a professor at the Yale School of Medicine who studies prison health care, said it is often difficult to gauge prison vaccination rates with certainty because inmates are often transferred, and many state prison systems do not disclose vaccine rates at all.
“If the best estimates are 50 percent, I’ll bet it’s lower,” Dr. Wang said. “And we’re not close to the mark. There’s no question in my mind, this hasn’t gone well.”
Ann Hinga Klein and
| United States › | United StatesOn May 21 | 14-day change | |
|---|---|---|---|
| New cases | 28,849 | –38% | |
| New deaths | 694 | –14% | |
| World › | WorldOn May 21 | 14-day change | |
|---|---|---|---|
| New cases | 288,911 | –30% | |
| New deaths | 5,055 | –14% | |
U.S. vaccinations ›
![]()
 Credit…James Estrin/The New York Times
Credit…James Estrin/The New York Times
When Covid-19 vaccines first became available, it was considered bad form or worse to travel to another city or state to get a shot. Florida, New York and other states banned the practice, limiting access to vaccines to their own residents and workers.
But now that vaccine supply is more abundant, many cities and states are making the shots available to all comers, even tourists. Next week, New York plans to open pop-up vaccination sites at seven airports in the state, including Kennedy International Airport and La Guardia Airport in New York City.
Offering the vaccine to travelers is an extension of the campaign to reach the unvaccinated that has been championed by the Biden administration and state and local officials. Gov. Andrew M. Cuomo of New York said the shots would be offered from Monday through Friday to people who were “traveling through or working at one of these airports or just happen to be passing through.”
New York City has set up sites at a number of places that are popular with tourists, including Times Square and the Bronx Zoo, as well as used buses and vans to bring vaccines into residential neighborhoods. Some visitors from other countries have gotten shots at pop-up sites set up at Grand Central Terminal and other transit hubs, according to the Metropolitan Transportation Authority, which runs the city’s subways.
Already, more than 700,000 out-of-towners have received at least one dose of their vaccine in New York City, according to the city’s Health Department. And Mayor Bill de Blasio has invited more, suggesting the abundance of doses in the city could help revive its stagnant tourist trade.
“This is a positive message to tourists: Come here. It’s safe. It’s a great place to be, and we’re going to take care of you,” Mr. de Blasio said this month while announcing plans to offer vaccinations at Brooklyn Bridge Park, the High Line and other gathering places. “We’re going to make sure you get vaccinated while you’re here with us.”
City and state agencies said they did not have statistics to show how effective offering vaccines might be as a lure to visitors. But Abbey Collins, a spokeswoman for the transportation authority, said the pop-up sites in the subways and at commuter railroad stations had been very successful.
Nearly 9,000 people have received Johnson & Johnson’s one-shot vaccine at those stations since May 12, Ms. Collins said. Part of the appeal, she admitted, was the complimentary seven-day MetroCard, a popular perk with short-term visitors.
“A lot of people come for the free MetroCard,” Ms. Collins said. “There’s also the ease and convenience of meeting people where they are.”
On Friday, one of the buses that were sent by the city to communities where vaccination rates were lagging was parked in Sunset Park, a lower-income Brooklyn neighborhood filled with immigrants. “People are lining up — it’s doing terrific,” said Patrick Gallahue, a spokesman for the city’s Health Department who was there. “The goal is to make it convenient as possible and to make it fun and to make it attractive to people.”
 Credit…Matt Slocum/Associated Press
Credit…Matt Slocum/Associated Press
As the threat from the coronavirus pandemic grew in early 2020, so did many governors’ executive powers. Without a federal plan, it fell to the states to issue lockdown and stay-at-home orders, mandate masks, and close schools and businesses.
Nearly 14 months later, with states moving to reopen amid a drastic drop in new cases, legislators have been asking about the current need for restrictions. And just how much sweeping authority do governors need to have during a public health emergency.
Voters in Pennsylvania this week became the first in the United States to help check an executive’s authority during an emergency period. The state’s Democratic governor, Tom Wolf, and its Republican-controlled legislature sparred over Mr. Wolf’s emergency actions, which included closing schools and many businesses, during the pandemic.
Two measures passed on Tuesday in Pennsylvania, both with about 54 percent approval. The state’s Constitution will be amended to end a governor’s emergency disaster declaration after 21 days. And lawmakers, with a simple majority, will be given the only authority to extend or end the emergency disaster declaration. The ballot questions had been pushed forward by Republican legislators.
At polling stations, many voters told Pennsylvania news outlets that they had been driven to vote in particular because of the ballot questions on executive power. Previously, a governor could issue a declaration for up to 90 days and extend it indefinitely and the legislature would need a two-thirds majority to stop a declaration. Mr. Wolf’s first 90-day virus emergency went into effect in March 2020, and his latest extension ends this week. But all of the remaining capacity restrictions on businesses and social gatherings in Pennsylvania end on May 31.
“We had a long period to see how the current system works, and there was some thought that we could to better,” Mr. Wolf said this week. “So I’m looking forward to working with the legislature to figure out how to make this work.”
In New Jersey, a Democrat-led legislature took the initial step this week to roll back dozens of Covid-related orders issued by Gov. Phil Murphy, also a Democrat. But the bill that was introduced also leaves the governor with expansive powers to apply new measures in an emergency. Mr. Murphy is one of two governors to keep an indoor mask mandate, even for vaccinated people; the other is Hawaii’s.
New executive orders related to the pandemic are still being announced. Gov. Greg Abbott of Texas, a Republican, said on Tuesday that counties, cities, public health authorities and local government officials in his state would be prohibited from requiring people to wear masks. His order came days after federal health officials announced new guidance that encouraged people who were fully vaccinated to forgo masks in most situations.
Democratic lawmakers in Connecticut, though, supported an extension this week of Gov. Ned Lamont’s expanded pandemic powers through mid-July. They were set to expire this week. Lawmakers argued that executive orders were still needed to manage the vaccine rollout and federal relief funds.
But perhaps no governor more than Andrew M. Cuomo, Democrat of New York, has faced a bigger rebuke in his use of emergency powers by a Democratic-controlled legislature. In February, the body curtailed Mr. Cuomo’s emergency powers, and in late April, it suspended some of his pandemic directives, including a rule that required New Yorkers to order food with their alcohol orders at bars and restaurants.
Mr. Cuomo also faces federal and state investigations, including one looking into his reporting of deaths at nursing home during the pandemic.
 Credit…Tom Jamieson for The New York Times
Credit…Tom Jamieson for The New York Times
Germany is banning most travel from Britain starting on Sunday amid concerns about the spread of a coronavirus variant first discovered in India, the German authorities said on Friday.
German citizens and residents of Germany will still be allowed to enter the country from Britain but will be required to quarantine for two weeks upon arrival, Germany’s public health institution said as it classified Britain as an area of concern because of the variant.
The move came just days after Britain reopened its museums and cinemas and resumed allowing indoor service in pubs and restaurants. Many people in Britain have been looking forward to traveling abroad in the coming months, and Spain is set to welcome visitors arriving from Britain without a coronavirus test starting on Monday.
Germany has classified the UK as an area of variant of concern, with effect from 23 May. Therefore a ban on transportation and entry into Germany applies from 23 May. Details and exceptions here: https://t.co/EmMuH1IuVo
— German Embassy London (@GermanEmbassy) May 21, 2021
The spread in Britain of the variant first detected in India, known as B.1.617, could serve as an early warning for other European countries that have relaxed restrictions. This month, the World Health Organization declared the mutation a “variant of concern,” and although scientists’ knowledge about it remains limited, it is believed to be more transmissible than the virus’s initial form.
Brazil, India and South Africa are among the dozen or so other countries that Germany considers areas of concern because of variants. As of Thursday, Britain has reported 3,424 cases of the variant first discovered in India, according to government data, up from 1,313 cases the previous week.
Dozens of nations, including European countries and the United States, suspended travel from Britain or imposed strict restrictions earlier in the pandemic amid concerns about the spread of a variant first detected in England.
The Office for National Statistics in the United Kingdom said on Friday that the percentage of people testing positive for the coronavirus in Britain had showed “early signs of a potential increase” in the week ending on May 15, although it said rates remained low compared with earlier this year. At its peak in late December, Britain recorded more than 81,000 cases, compared with about 2,000 this month.
The country’s inoculation campaign is continuing apace, with an increased focus on second doses in an effort to thwart the sort of spikes that led to restrictions imposed this year.
More than 37 million people, or 56 percent of the country’s population, have received a first dose of a Covid-19 vaccine in Britain. Yet most people under age 30 have yet to receive a dose, and less than a third of the population has been fully vaccinated. Health Minister Matt Hancock said on Saturday that people over 32 could now book an appointment.
Prime Minister Boris Johnson has vowed to proceed with a plan to lift all restrictions by June 21, although scientists have warned that the spread of the B.1.617 variant could delay such plans. Most cases of the variant have been found in northwestern England, with some in London.
In Germany, the restrictions on travel from Britain come as outdoor service resumed on Friday in cafes, restaurants and beer gardens after months of closure. Chancellor Angela Merkel urged people to “treat these opportunities very responsibly.”
“The virus,” she said, “has not disappeared.”
 Credit…Amira Karaoud/Reuters
Credit…Amira Karaoud/Reuters
Several Covid-19 mitigation measures — including improving ventilation, requiring adults to wear face masks and conducting frequent surveillance testing — can help schools stay open and students remain safe, two new studies suggest.
The studies, which were published on Friday, come as many school districts are drawing up their plans for the fall. They also follow the Centers for Disease Control and Prevention guidance that all schools teaching students from kindergarten through grade 12 should continue to have mask-wearing policies through the end of the 2020-21 school year, after the agency’s recent move to allow for vaccinated people to forgo wearing masks indoors. The agency also kept in place its suggestions to observe physical distancing and to test for coronavirus infections.
In one of the new studies, researchers from the C.D.C. and the Georgia Department of Public Health surveyed 169 elementary schools in Georgia that offered in-person learning in the fall. The group asked the schools about their pandemic responses and collected data on the coronavirus cases detected between Nov. 16 and Dec. 11, before Covid-19 vaccines were available in the United States.
The researchers found that the incidence of the virus was 35 percent lower in schools that had improved their ventilation — by opening windows or doors, or using fans — than in schools that did not adopt these practices. In schools that combined better ventilation with air filtration — through the use of HEPA filters, for instance — case rates were 48 percent lower.
Requiring all teachers and staff members to wear masks reduced the incidence of the virus by 37 percent, the researchers found. Schools that required students to wear masks had a 21-percent-lower incidence of the virus, but that reduction was not statistically significant, the scientists found. That may be a result of the fact that adults are more likely to transmit the virus than children are, or simply because of a small sample size.
“Because universal and correct use of masks can reduce SARS-CoV-2 transmission and is a relatively low-cost and easily implemented strategy, findings in this report suggest universal and correct mask use is an important Covid-19 prevention strategy in schools as part of a multicomponent approach,” the researchers write.
A second study, led by researchers at the Utah Department of Health and the University of Utah, tracked the implementation of two coronavirus screening programs in the state’s schools. One program, which was established in January 2021, allowed schools with outbreaks to conduct schoolwide testing instead of shifting to remote learning.
“Schools could either do what they had been doing in the fall, which was switch to remote for a two-week period to interrupt transmission chains, or it could test everyone,” said Dr. Adam Hersh, one of the study’s authors and an expert in pediatric infectious diseases at the University of Utah. “And those who tested negative could return to in-person learning and those who tested positive obviously would be isolated.”
A second testing program required students to be tested for the coronavirus every 14 days in order to participate in sports or other extracurricular activities. Both initiatives relied on rapid antigen tests, which are less sensitive, but cheaper and faster, than the standard P.C.R. tests.
This year, between Jan. 4 and March 20, 28 high schools in the state reported sizable outbreaks. Fifteen schools moved to remote instruction for two weeks, while the other 13 conducted surveillance testing instead. Of the 13,809 students who were tested as part of this screening, just 0.7 percent tested positive, the scientists reported. All 13 schools remained open.
“From a public health standpoint, it’s a huge success,” said Kendra Babitz, the coronavirus testing coordinator at the Utah Department of Health and one of the study’s authors. “Testing is and should be a mitigation strategy that schools are using to prevent transmission of SARS-CoV-2 in the school setting,” she added, referring to the virus that causes Covid-19.
Over the course of the winter, 95 percent of school athletic events took place as scheduled, the researchers found, although they did not compare that figure with a control group of schools without screening programs. “That’s in range with what happens in normal season,” Dr. Hersh said. “The show was able to go on.”
IN CASE YOU MISSED IT
 Credit…Emily Elconin for The New York Times
Credit…Emily Elconin for The New York Times
After almost a year and a half of sickness, there is a chance that the coronavirus pandemic could be entering a permanent retreat in the United States. The country is adding fewer than 30,000 cases a day for the first time since June, and deaths are as low as they’ve been since July. Nearly everywhere, the outlook is improving.
More than 60 percent of American adults have received at least one vaccine shot, and though the pace has slowed, the share is still growing by about two percentage points per week.
“In the United States, there is now an excellent chance that the retreat is permanent,” David Leonhardt wrote in his Morning newsletter on Friday.
The share of coronavirus tests coming back positive has fallen below 3 percent for the first time since widespread testing began, and the number of hospitalized patients has fallen to the lowest point in 11 months, Dr. Eric Topol of the Scripps Research Translational Institute noted. For the first time since March 5 of last year, San Francisco General Hospital yesterday had no Covid-19 patients — “a truly momentous day,” Dr. Vivek Jain said.
Michigan, the state that reported one of the largest surges in the spring, has rapidly improved. About 1,600 cases are being identified there each day, compared with about 7,800 cases a day in mid-April.
Important caveats remain: Covid-19 is still especially dangerous in communities with low vaccination rates, and it’s becoming clearer that getting vaccines into these communities is crucial in continuing to curb the virus.
Around the world, however, the situation is not as encouraging although it is slowly getting better. Most low- and middle-income countries are struggling because they lack access to vaccines. In Africa, only 1.4 percent of people have received a shot, according Oxford University’s Our World in Data project, and the numbers are only modestly higher in much of Latin America, the Middle East and Southeast Asia. Even the European Union struggled until recently to ramp up vaccinations.
Here’s what else you may have missed:
 Credit…Max Whittaker for The New York Times
Credit…Max Whittaker for The New York Times
For more than 400 colleges and universities, it’s being billed as the ticket to a normal year on campus: Require all students to be vaccinated for the coronavirus before they can matriculate next fall.
From just one university in March, to a dozen by the first week of April, the floodgates have now opened with at least 403 colleges announcing a mandatory vaccine.
Yet a look at the geographic spread of the universities reveals a stark, if unsurprising, divide: The overwhelming majority of the colleges that are requiring the immunization are in blue states.
Only 32 — 8 percent — are in states that voted for Donald Trump, according to a tracker created by the Chronicle of Higher Education. Seven of those were added Friday, when Indiana University and its satellite campuses became rare public universities in Republican-controlled states mandating vaccines.
With many colleges facing falling enrollments and financial pressure, the decision whether to require vaccinations can have huge consequences. Particularly in Republican-controlled states, college presidents are weighing a delicate equation – part safety, part politics, part peer pressure and part economic self-interest.
On weekly conference calls with presidents of other universities, the subject has become a frequent topic of discussion, said Katie Conboy, the president of Saint Mary’s College, a private all-women college in Indiana.
“People are waiting for a tipping point. They’re not saying, we’re going to be out on the leading edge of this, but we are watching and waiting and hoping it will make sense for us,” said Ms. Conboy.
 Credit…Haitham Imad/EPA, via Shutterstock
Credit…Haitham Imad/EPA, via Shutterstock
Health officials and international aid groups are watching to see whether nearly two weeks of fighting between Israel and Hamas militants led to a wave of new coronavirus cases in Gaza.
The United Nations warned on Monday, at the start of the second week of fighting, of a potential surge of new cases as tens of thousands of Gazans took shelter in 50 U.N.-run schools. A cease-fire was declared on Friday.
“The schools were overcrowded and there was basically no social distancing in them,” said Dr. Majdi Dhair, director of preventive medicine for the Palestinian health ministry in Gaza. “If someone was sick in any one school, that person could have infected everyone around them.”
A majority of Gazans most likely hunkered down in their homes during the two weeks of fighting and had less contact than usual with others, which could ultimately temper the size of any new outbreak, Dr. Dhair said. It would take several days for the case data to show the extent of a possible spike.
The only laboratory in the Gaza Strip that processes coronavirus tests was damaged in an Israeli airstrike, but it reopened on Thursday. In the Rimal clinic in Gaza City, windows were replaced, rooms were cleaned and the machines, which were lightly damaged, were examined and approved for use, Dr. Dhair said.
The lab processed 547 tests on Thursday and Friday, of which 202 were positive.
Michael Lynk, the U.N. special rapporteur on Palestinian human rights, said preserving vaccine access was crucial in Gaza, where inoculations were temporarily halted by the fighting. Gaza remains highly vulnerable to an outbreak, with less than 4 percent of its population fully or partially vaccinated. That’s far below the 60 percent in Israel, one of the highest rates in the world.
“Israel is the occupying power in the West Bank and in Gaza, and it has very strict obligations,” Mr. Lynk said. He said the United Nations has reminded Israel of those obligations.
Getting vaccine supplies into the territory has been hard enough. Gaza lacks funds to buy the doses, and although the territory is supposed to get aid from Covax, the global vaccine sharing program has been slow to deliver them. Recently, the Chinese government has said that it would donate doses to the U.N. agency that focuses on aid to Palestinian refugees.
“If there was a surge again, it would require a huge rapid infusion of international donors to find vaccines going into Gaza, and making sure you have enough trained health care staff to administer mass inoculation,” Mr. Lynk said.
Israeli bombs have damaged several hospitals and clinics, hindering an already crumbling health care system, and it is not clear how long it will take to repair them. Fresh water and sewage systems have also been damaged, which could lead to disease outbreaks.
After a surge in cases in April, which was blamed mostly on the highly transmissible coronavirus variant first identified in Britain, new cases in Gaza had recently fallen. As of Thursday, the territory, with more than two million people, reported 26 critical cases and 68 serious cases.
 Credit…Gabby Jones for The New York Times
Credit…Gabby Jones for The New York Times
Billions of dollars in Covid aid cushioned financial losses caused by the pandemic at some of the largest hospital chains in the nation. But those bailouts also helped to sustain the big chains’ spending sprees as they expanded even more by scooping up weakened competitors and doctors’ practices.
More consolidation by several major hospital systems enhanced their market prowess in many regions of the United States, even as rural hospitals and underserved communities were overwhelmed with Covid-19 patients and struggled to stay afloat.
The buying spree is likely to prompt further debate and scrutiny of the Provider Relief Fund, a package of $178 billion in congressional aid that drew sharp criticism early on for allocating so much to the wealthiest hospital systems, and that had no limits on mergers and acquisitions.
The Biden administration is now weighing which hospitals and health providers will get the remaining $25 billion.
“It was not the intent to be a capital infusion to the largest and most financially stable providers to allow them to simply grow their slice of market share,” Representative Katie Porter, Democrat of California, said. She is calling for hearings and for the Federal Trade Commission to review whether the funds have been properly used for patient care and operations.