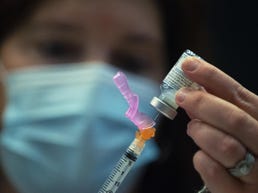
Avoid pain medication before getting the COVID-19 vaccine, but they are “perfectly fine” according to experts
Headache, fever, body aches and chills.
While these are perfectly normal side effects of the COVID-19 vaccine – and a good sign that your immune system is working – they can be uncomfortable.
To minimize the discomfort, some Americans may turn to pain relievers such as acetaminophen or ibuprofen. Others fear that these drugs could make the vaccine less effective.
Studies on the subject are sparse and inconsistent, but the Centers for Disease Control and Prevention and the World Health Organization both advise against the preventive use of pain relievers.However, allow them if symptoms develop afterward.
In a study published in the peer-reviewed Journal of Virology, researchers found that nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can reduce the production of antibodies and affect other aspects of the immune response to SARS-CoV-2, the virus that causes COVID-19 .
Researchers said the study’s results increased the possibility that pain relievers like ibuprofen could alter the immune response to the COVID-19 vaccine.
Dr. Colleen Kelley, an associate professor of medicine at Emory University School of Medicine who was not involved in the study, speculates that this could be caused by lowering the inflammation caused by the immune system.
“The immune system creates a response through controlled inflammation. (Painkillers) can reduce the production of inflammatory mediators, ”she said. “So this is the potential mechanism for a decreased immune response to vaccinations when you take these drugs.”
According to Dr. Marian Michaels, a member of the COVID-19 Vaccine Advisory Board at the University of Pittsburgh Medical Center, studies have shown that the immune system reacts differently to the COVID-19 vaccine than it does to natural infections.
“We believe the (immune) response to the vaccine is actually a better response than the wild-type virus with COVID-19,” said Michaels, who is also a pediatric infectious disease doctor at UPMC Children’s Hospital in Pittsburgh. “For this reason, we recommend that someone who has had an infection in the past continues to receive the vaccine.”
‘This is fantastic’:Mass vaccination clinics are playing a key role in ending the COVID-19 pandemic
A 2016 study by Duke University looked at the effectiveness of various vaccines in children and found that those who took pain medication before they got their regularly scheduled admissions had fewer antibodies than those who didn’t.
The few studies on pain medication and vaccines, however, aren’t robust enough to draw conclusions, experts say, as the children in the 2016 study who took pain medication and showed fewer antibodies still had a sufficient immune response to provide protection.
There is no data showing a decreased immune response when the drugs are taken after vaccination to treat side effects, Kelley added.
“Look actively at it”:Do travelers need a COVID-19 negative test to board flights within the US? The CDC says it is being considered
“It’s perfectly fine to take NSAIDs or Tylenol if you feel unwell after vaccination,” said Kelley. “The symptoms you are experiencing indicate that your immune system is working normally and that the immune response is continuing.”
Michaels notes that neither the Pfizer BioNTech nor the Moderna COVID-19 studies banned study participants from taking pain relievers and that efficacy rates were still above 95%.
“Although I don’t have the exact number of people in the research study … I’m sure some of them took acetaminophen or ibuprofen because 70% had mild (vaccine side effects),” she said. “And yet there was still an immunological response.”
Follow Adrianna Rodriguez on Twitter: @AdriannaUSAT.
US TODAY health and patient safety coverage is made possible in part by a grant from the Masimo Foundation for Ethics, Innovation and Competition in Healthcare. The Masimo Foundation does not provide any editorial contributions.